Boram Lee1, O.-Jin Kwon1, Joo-Hee Kim2,3, Jung Won Kang4, Tae-Hun Kim5, Seunghoon Lee4, Jungeun Kim6, Ae-Ran Kim7, So Young Jung7, Hyo-Ju Park7 and Sun-Mi Choi 8,9 (Hindawi Evidence-Based Complementary and Alternative Medicine Volume 2022, Article ID 2581041, 11 pages
- 1 KM Science Research Division, Korea Institute of Oriental Medicine, Daejeon, Republic of Korea
- 2 Department of Acupuncture and Moxibustion Medicine, College of Korean Medicine, Sangji University, Wonju, Gangwon-do, Republic of Korea
- 3 Research Institute of Korean Medicine, Sangji University, Gangwon-do, Republic of Korea
- 4 Department of Acupuncture and Moxibustion, College of Korean Medicine, Kyung Hee University, Seoul, Republic of Korea
- 5 Korean Medicine Clinical Trial Center, Korean Medicine Hospital, Kyung Hee University, Seoul, Republic of Korea
- 6 Acupuncture, Moxibustion & Meridian Research Group, Korea Institute of Oriental Medicine, Daejeon, Republic of Korea
- 7 Clinical Research Coordinating Team, Korea Institute of Oriental Medicine, Yuseong-daero 1672, Yuseong-gu, Daejeon, Republic of Korea
- 8 KM Data Division, Korea Institute of Oriental Medicine, Daejeon, Republic of Korea
- 9 Korean Convergence Medical Science, University of Science & Technology (UST), Daejeon, Republic of Korea
1. Introduction
Functional dyspepsia (FD) refers to the presence of one or more symptoms of epigastric pain, epigastric burning, early satiation, and postprandial fullness without organic, metabolic, or systemic disease. The symptoms are severe enough to interfere with usual activities over the last 3 months after an onset of at least 6 months prior [1]. The prevalence is reported to be very high worldwide, 10–21%, causing a global burden [2, 3]. It is not a life-threatening disease, but it reduces sufferers’ quality of life with chronic and repetitive symptoms. The direct and indirect costs of FD to patients have been estimated to be $18.4 billion for the US population, imposing a significant economic burden on the healthcare system [4].
According to the American College of Gastroenterology and the Canadian Association of Gastroenterology guidelines on dyspepsia, Helicobacter pylori eradication, proton pump inhibitors (PPIs), tricyclic antidepressants, and prokinetic therapy are recommended for patients with FD [5].
However, because of the heterogeneous and diverse characteristics of FD symptoms [6] and the possible side effects of conventional medication, including extrapyramidal reactions [7], almost 50% of patients were found to use complementary and integrative medicine (CIM) such as acupuncture and herbal medicine [8].
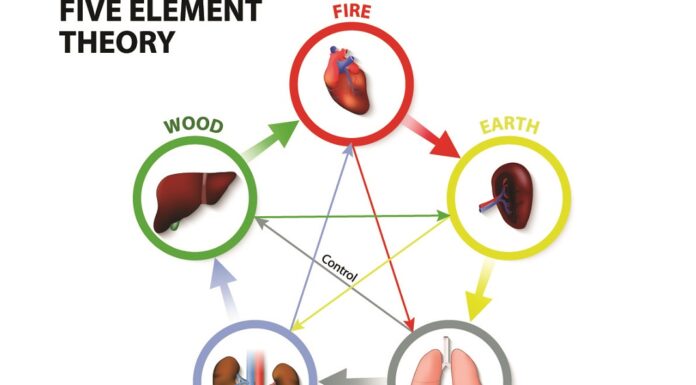
Acupuncture is one of the most popular CIM treatments, and it is used for the treatment and management of various diseases. According to the data provided by the Health Insurance Review & Assessment Service of South Korea in 2020, FD is a common disease that ranks in the top 8 in terms of the number of patients visiting Korean medicine (KM) clinics [9], and acupuncture is actively used to treat FDin clinical settings. Saam (Sa-Ahm) acupuncture is a unique acupuncture method of traditional KM, believed to have been developed in the mid-17th century by a Korean Buddhist monk named “Saam.” It differs from other Chinese acupuncture methods in that it uses the five shu points, located on the distal upper and lower limbs, belonging to the self-meridian and other meridians according to the cold-heat and deficiency-excess pattern identification [10, 11]. Therefore, the therapeutic purpose of Saam acupuncture is to control the balance between the five elements and the cold-heat and deficiency excess pattern balance between the viscera and bowels [12].
According to surveys conducted among KM clinical doctors, acupuncture is used most often on FD patients in clinical settings, with body and Saam acupuncture used most frequently [13]. However, although studies related to acupuncture for the treatment of FD are being actively conducted, mainly in China [14–16], there have been no clinical trials on the actual effect of Saam acupuncture, which has been used in the KM clinical field on FD. Therefore, we aimed to generate basic evidence regarding the preliminary effectiveness and safety of Saam acupuncture on FD patients and to evaluate the feasibility of a confirmatory clinical trial.
2. Methods
- 2.1. Study Design. .is trial was a pilot, pragmatic, assessor-blinded randomized controlled trial that examined the feasibility and preliminary effectiveness and safety of Saam acupuncture for treating FD patients. A total of 24 patients were randomly assigned to a 4-week acupuncture plus usual care group or a usual care group. It was conducted from March 2011 to March 2013 at Daejeon KM Hospital of Daejeon University in the Republic of Korea in accordance with the Declaration of Helsinki. Ethical approval was obtained from the institutional review board (approval number: djomc-55). In addition, the protocol was registered in the web database of the Clinical Research Information Service (registration number: KCT0000164). The trial was designed and reported following the Consolidated Standards of Reporting Trials (CONSORT) and the Standards for Reporting Interventions in Clinical Trials of Acupuncture (STRICTA) recommendations [17, 18].
- 2.2. Participants. Among those who agreed to participate in the trial and voluntarily signed an informed consent form after listening to a clear explanation of the purpose and characteristics of the clinical trial, those who met the following conditions were included: (1) those aged between 20 and 65, (2) those who were diagnosed with FD according to the ROME III criteria [19] (having at least one symptom among the following: postprandial fullness, early satiety, epigastric burning, and epigastric pain for the past 3 months with symptom onset at least 6 months before the screening visit, without any evidence of structural disease that was likely to explain the symptoms on upper gastrointestinal endoscopy), and (3) those with a dyspepsia symptom severity score of at least 40 points on a 0–100 visual analog scale (VAS) during the past week at the time of the screening visit. Participants who met the following conditions were excluded: (1) those who were at risk of gastrointestinal motility stimulus due to gastrointestinal bleeding, mechanical intestinal obstruction, or perforation; (2) those having alarm symptoms such as severe weight loss, melena, dysphagia, repeated vomiting, anemia, jaundice, abdominal mass, or ascites; (3) those having received KM treatment for the treatment of FD during the last 4 weeks; (4) those having undergone a gastrointestinal surgery except for appendectomy in the past or those who had a disease such as cholangitis or pancreatitis; (5) those having been judged not appropriate for participating in this clinical trial due to severe cardiovascular disease, severe neurological disease, acute or chronic liver disease such as liver cancer or liver cirrhosis, malignant tumor, chronic lung and respiratory disease, poorly controlled hypertension or diabetes, drug addiction, alcoholism, chronic renal failure, active tuberculosis, other infectious diseases, mental disease, or a diet disorder that occurred during the last year; (6) those having taken medications that could affect the results of the trial as a conventional FD treatment or by causing indigestion as side effects, including PPIs, H2-receptor antagonists, corticosteroids, and nonsteroidal anti-inflammatory drugs (NSAIDs), within the last 1 month as self-reported and confirmed prescription; (7) those having hemorrhagic disease or taking anticoagulant drugs (except for aspirin); (8) those having experienced a hypersensitivity reaction after a previous acupuncture treatment; (9) those being held in group facilities such as social welfare facilities; (10) women who were pregnant or lactating or planned to become pregnant during the trial period; (11) those having participated in other clinical trials during the past 3 months; and (12) those judged inappropriate for participating in this trial by the investigators.
- 2.3. Randomization and Blinding. An independent statistician generated a random sequence number using SAS version 9.1.3 software (SAS Institute Inc., Cary, NC, USA), with an allocation ratio of 1 :1 to each group. A block randomization method was used with a block size of 4, without stratification. Opaque envelopes with random assignment codes were sealed and stored in a double-locked cabinet. For the participants who met the inclusion criteria and did not meet the exclusion criteria, the investigators completed all evaluations at the baseline visit and then opened the opaque sealed envelopes in order in front of the participants and assigned them to each group. Although blinding was not possible for the clinicians conducting the acupuncture treatment or the study participants due to the nature of the study design, the outcome assessor and data analyst were blinded to the group allocation during the trial period.
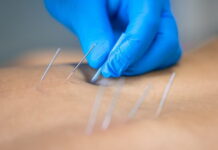
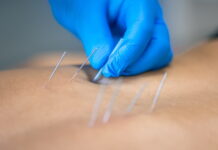
- 2.4. Intervention. When the inclusion and exclusion criteria were reviewed at the screening visit, and it was judged by the investigators that participation in the clinical trial was appropriate, the participants were enrolled in this clinical trial within 10 days of the screening visit and randomly assigned to the acupuncture plus usual care group or the usual care group. In the acupuncture group, individualized Saam acupuncture treatment was performed, based on its use in the KM clinical field [11–13], with reference to the consensus among five KM specialists, textbooks on acupuncture and moxibustion [20], and external expert advice. Saam acupuncture, based on The Classic of Difficult Issues (Nanjing), was combined with the engendering and restraining relationship between the five elements. A total of four acupuncture points located in distal limbs were prescribed by selecting two acupuncture points from the self and other meridians, respectively, according to the cold-heat and deficiency-excess pattern [21] (Supplement 1). Individualized Saam acupuncture consisting of four acupuncture points was conducted based on the judgment of a KM specialist with more than 5 years of clinical experience and more than 6 years of regular medical education, considering the FD symptoms and systemic symptoms that each patient complained of, according to the principles of a pragmatic clinical trial. In accordance with the principles of the Saam acupuncture method, acupuncture was performed on the left side of men and the right side of women. Disposable sterile acupuncture needles (0.25 × 30 mm; Dong Bang Acupuncture Inc., Seoul, Republic of Korea) were inserted into each acupuncture point at a depth of 0.2–1.5 cun and maintained for 20 min. .e manipulation technique was applied until the local “de qi” sensation (soreness, numbness, heaviness, and distention) was achieved. Acupuncture treatment was performed three times a week for 4 weeks, a total of 12 times, and according to the principles of pragmatic clinical trials, the acupuncture therapist was allowed to communicate with the participants about the daily management and treatment of symptoms during the treatment period. Participants who did not receive three or more consecutive acupuncture treatments or received fewer than 10 out of 12 treatments in the acupuncture group were dropped out. Except for the KM treatment, all kinds of treatment for FD, such as over-the-counter drugs and prescription drugs, were allowed, and all concomitant treatments were recorded in a case report form (CRF). However, treatments for symptoms other than FD that could affect dyspepsia symptoms, such as long-term NSAID use for arthritis, were prohibited during the clinical trial period under the judgment of the investigators. Education on FD lifestyle management was conducted using a brochure. The usual care group received the same treatment as the acupuncture group except the acupuncture treatment.
- 2.5. Outcome Measures. The primary outcome measure was feasibility outcomes to examine the feasibility of a confirmatory clinical trial, including recruitment rate (percentage of the number of enrolled participants to the total number of screening participants), completion rate (percentage of the number of participants who completed the clinical trial without dropping out to the total number of enrolled participants), attrition rate, and adherence rate of acupuncture (percentage of participants, after excluding those who did not receive three or more consecutive acupuncture treatments or who received fewer than 10 out of 12 treatments, in the acupuncture group). The preliminary evaluation of participant response to the intervention was tested using gastrointestinal symptom (GIS), FD-related quality of life (FD-QoL), VAS, 3-level version of the EuroQol-5 Dimensions (EQ-5D-3L), and patient global assessment (PGA) scores at Weeks 4, 8, and 12. .e GIS questionnaire is a validated, self-rating 10-item questionnaire assessing dyspepsia-specific symptoms. .e 10 items include nausea, vomiting, bloating, abdominal cramps, early satiety, acidic eructation/heartburn, sickness, loss of appetite, retrosternal discomfort, and epigastric/upper abdominal pain and are evaluated on a 5-point Likert scale (0–4) [22, 23], with a higher score indicating more severe indigestion. The GIS scores were measured at Weeks 0 (baseline visit), 4 (treatment termination), 8 (follow-up after final intervention), and 12 (second follow-up after final intervention). With 21 items, the FD-QoL questionnaire assesses four dimensions of patients, including psychological status, role-functional status, eating status, and liveliness status [24]. Each item is evaluated on a 5-point Likert scale (0–4), with a higher score indicating lower quality of life. In addition, the VAS with a measurement range of 0 (no discomfort) to 100 (most painful condition) was performed to evaluate the overall discomfort caused by FD. .e average daily symptoms for the last week were investigated. The EQ-5D-3L assesses health-related quality of life, including mobility, personal care, usual activities, pain/discomfort, and anxiety/depression [25, 26]. We used a validated Korean EQ-5D-3L questionnaire and calculated the quality-adjusted life year from the score. The PGA was used to evaluate how well the patients’ FD symptoms improved compared to before treatment. The patients responded to the overall improvement after treatment using a 5-point scale, ranging from “much improved” to “much worse.” In addition, we evaluated the safety of the intervention by investigating adverse events (AEs) that occurred during the study period through medical examinations and the participants’ self-reports. .e severity and causal relationships between the AEs and the intervention were recorded in the CRFs.
- 2.6. Sample Size and Statistical Analysis. This study was the first preliminary clinical trial to evaluate the effectiveness, safety, and study feasibility of Saam acupuncture for FD patients. Due to a lack of previous studies, we could not find adequate references for a sample size calculation, and therefore, this preliminary study was undertaken to provide a reference for this calculation. According to a study that recommended a minimum of 12 participants per group for a pilot study [27], we aimed to recruit a total of 24 participants, with 12 participants per group for assessing feasibility. A statistician (OJK) independent of the intervention and evaluation conducted all statistical analyses using SAS version 9.4 software (SAS Institute Inc.). An intention-to treat analysis method was used that included all participants who received acupuncture treatment and an assessment at least once after randomization. After checking the satisfaction of the normality assumption, a two-sided test with a significance level of 0.05 was performed using an analysis of covariance with the baseline as the covariate and the treatment group as the fixed factor. In addition, the differences before and after the treatment within each group were verified by a paired t-test. Multiple imputations were applied for missing values. A repeated-measures analysis of variance was performed to test the difference in the trend change by visits between each group.
References
- [1] V. Stanghellini, F. K. L. Chan, W. L. Hasler et al., “Gastroduodenal disorders,” Gastroenterology, vol. 150, no. 6, pp. 1380–1392, 2016.
- [2] A. C. Ford, A. Marwaha, R. Sood, and P. Moayyedi, “Global prevalence of, and risk factors for, uninvestigated dyspepsia: a meta-analysis,” Gut, vol. 64, no. 7, pp. 1049–1057, 2015.
- [3] I. Aziz, O. S. Palsson, H. T¨ornblom, A. D. Sperber, W. E. Whitehead, and M. Simr´en, “Epidemiology, clinical characteristics, and associations for symptom-based Rome IV functional dyspepsia in adults in the USA, Canada, and the UK: a cross-sectional population-based study,” =e lancet Gastroenterology & hepatology, vol. 3, no. 4, pp. 252–262, 2018.
- [4] B. E. Lacy, K. T. Weiser, A. T. Kennedy, M. D. Crowell, and N. J. Talley, “Functional dyspepsia: the economic impact to patients,” Alimentary Pharmacology and =erapeutics, vol. 38, no. 2, pp. 170–177, 2013.
- [5] P. M. Moayyedi, B. E. Lacy, C. N. Andrews, R. A. Enns, C. W. Howden, and N. Vakil, “ACG and CAG clinical guideline: management of dyspepsia,” American Journal of Gastroenterology, vol. 112, no. 7, pp. 988–1013, 2017.
- [6] M. Camilleri and V. Stanghellini, “Current management strategies and emerging treatments for functional dyspepsia,” Nature Reviews Gastroenterology & Hepatology, vol. 10, no. 3, pp. 187–194, 2013.
- [7] E. M. M. Quigley, “Prokinetics in the management of functional gastrointestinal disorders,” Journal of neurogastroenterology and motility, vol. 21, no. 3, pp. 330–336, 2015.
- [8] E. Lahner, S. Bellentani, R. D. Bastiani et al., “A survey of pharmacological and nonpharmacological treatment of functional gastrointestinal disorders,” United European gastroenterology journal, vol. 1, no. 5, pp. 385–393, 2013.
- [9] Health Insurance Review & Assessment Service, “Statistics of frequent diseases,” 2021, http://opendata.hira.or.kr/op/opc/olapHifrqSickInfo.do.
- [10] M. Park and S. Kim, “A modern clinical approach of the traditional Korean Saam acupuncture,” Evidence-based complementary and alternative medicine, vol. 2015, Article ID 703439, 8 pages, 2015.
- [11] S.-Y. Kim, S. H. Hong, J.-W. Park et al., “Analysis of acupuncture diagnostic decision from the clinical information of a functional dyspepsia patient,” Integrative Medicine Research, vol. 9, 2020.
- [12] D. Jang, K.-C. Oh, E.-S. Jung et al., “Diversity of acupuncture point selections according to the acupuncture styles and their relations to theoretical elements in traditional asian medicine: a data-mining-based literature study,” Journal of Clinical Medicine, vol. 10, 2021.
- [13] National Institute for Korean Medicine, “Guideline center for Korean medicine and the society of internal Korean medicine,” Korean Medicine Clinical Practice Guideline for Functional Dyspepsia, Koonja Publishing Inc., Seoul, South Korea, 2017.
- [14] K.-N. Kim, S.-Y. Chung, and S.-H. Cho, “Efficacy of acupuncture treatment for functional dyspepsia: a systematic review and meta-analysis,” Complementary =erapies in Medicine, vol. 23, no. 6, pp. 759–766, 2015.
- [15] C.-Y. Kwon, S.-J. Ko, B. Lee, J. M. Cha, J. Y. Yoon, and J.-W. Park, “Acupuncture as an add-on treatment for functional dyspepsia: a systematic review and meta-analysis,” Frontiers of Medicine, vol. 8, 2021.
- [16] B. Pang, T. Jiang, Y.-H. Du et al., “Acupuncture for functional dyspepsia: what strength does it have? A systematic review and meta-analysis of randomized controlled trials,” Evidence based Complementary and Alternative Medicine, vol. 2016, Article ID 3862916, 17 pages, 2016.
- [17] H. MacPherson, D. G. Altman, R. Hammerschlag et al., “Revised STandards for reporting interventions in clinical trials of acupuncture (STRICTA): extending the CONSORT statement,” Journal of alternative and complementary medicine, vol. 16, 2010.
- [18] D. Moher, S. Hopewell, K. F. Schulz et al., “CONSORT 2010 explanation and elaboration: updated guidelines for reporting parallel group randomised trials,” BMJ, vol. 340, 2010.
- [19] J. Tack, N. J. Talley, M. Camilleri et al., “Functional gastroduodenal disorders,” Gastroenterology, vol. 130, no. 5, pp. 1466–1479, 2006.
- [20] “Acupuncture and Moxibustion medicine society textbook compilation committee,” =e Acupuncture and Moxibustion Medicine, Jipmoondang Publishing Co., Seoul, South Korea, 2012.
- [21] Y.-O. Jung, D.-H. Lee, and S.-W. Ahn, “A research for tradition and identity of Saam acupuncture method,” Korean Journal of Acupunct, vol. 29, pp. 537–553, 2012.
- [22] A. Madisch, G. Holtmann, G. Mayr, B. Vinson, and J. Hotz, “Treatment of functional dyspepsia with a herbal preparation,” Digestion, vol. 69, no. 1, pp. 45–52, 2004.
- [23] G. Holtmann, J. Gschossmann, P. Mayr, and N. J. Talley, “A randomized placebo-controlled trial of simethicone and cisapride for the treatment of patients with functional dyspepsia,” Alimentary Pharmacology and =erapeutics, vol. 16, no. 9, pp. 1641–1648, 2002.
- [24] E.-H. Lee, K.-B. Hahm, J. H. Lee et al., “Development and validation of a functional dyspepsia-related quality of life (FDQOL) scale in South Korea,” Journal of Gastroenterology and Hepatology, vol. 21, no. 1, pp. 268–274, 2006.
- [25] M.-H. Kim, Y.-S. Cho, W.-S. Uhm, S. Kim, and S.-C. Bae, “Cross-cultural adaptation and validation of the Korean version of the EQ-5D in patients with rheumatic diseases,” Quality of Life Research, vol. 14, no. 5, pp. 1401–1406, 2005.
- [26] R. Rabin and F. d. Charro, “EQ-SD: a measure of health status from the EuroQol Group,” Annals of Medicine, vol. 33, no. 5, pp. 337–343, 2001.
- [27] S. A. Julious, “Sample size of 12 per group rule of thumb for a pilot study,” Pharmaceutical Statistics, vol. 4, no. 4, pp. 287–291, 2005.